Türkçede Kron olarak telaffuz edilen bu hastalığın Latincede “Crohn’s disease” yani Crohn Hastalığı olarak bilinir. Özellikle karnın sağ alt köşesinde ağrı ile kendini ortaya koyar.
Bu hastalığın adı ilk olarak 1932 yılında Burrill Crohn ve arkadaşları tarafından kronik inflamatuar ileum hastalığı hakkında yayınlanan çalışmaları ile duyuruldu ve tıbbi literatürlere geçti.
CROHN Hastalığı nedir?
CROHN Hastalığı (CH), sindirim sisteminin dudaklardan itibaren anal halkasına kadar herhangi bir bölgeyi etkileyebilen tam kat kronik inflamatuar bir hastalıktır.
Daha çok Kuzey Amerika ve Kuzey Avrupa ülkelerinde görülmektedir. Her yıl 100.000 insandan 5’inde görülür. Özellikle son 40 yıl içerisinde vaka sayısında artış görülmektedir.
Erkeklere göre bayanlarda daha fazla görülür özellikle 25-40 yaşları arasında daha yoğun olduğu tespit edilmiştir. Hastalığın ikinci zirve yaptığı dönem ise 70’li yaşlardadır. CROHN Hastalığı özellikle Aşkenaz Yahudi topluluklarında yaygındır.
Sebepleri
CH nedenleri henüz tam olarak bilinmemekle birlikte (ideopatik) genetik ve çevresel faktörlerin karmaşık etkileşiminin rol oynadığı düşünülmektedir. Her ne kadar CROHN Hastalığı ile kronik infeksiyon arasından çok sayıda benzer özellik olsa da bugüne kadar hiçbir etken organizma gösterilmemiştir.
Mycobacterium paratuberculosis enfeksiyonundan kaynaklanan ve sığırlarda görülen Johne hastalığı ile benzer ekenlerin olduğu düşünülmektedir. Rafine gıdaların tüketilmesi, sigara, genetik yatkınlık (NOD2/CARD15, tek yumurta ikizler)
Patoloji ve Patogenez
Artan mukoza geçirgenliği sonucunda luminal antigenlerin geçişi ile hücre aracılı inflamatuar yanıtın uyarılmasına bağlı olduğu düşünülmektedir. Bu durum lokal ve sistemik inflamatuvar yanıtlara yol açan proinflamatuar sitokinlerin (il2 interleukin 2, TNF tümör nekrotizan faktör) salımına bağlı olduğu göterilmiştir. Bu mekanizma süpresör T hücrelerindeki bir defekte bağlı olduğu ileri sürülmüştür.
Terminal ileum nedir ?
Terminal ileum ince barsağın (small intestine) en son kısmıdır. Uzunluğu 3-4 cm’dir. Terminal ileumun uç tarafında ileoçekal sfinkter yer alır. Bu sifinkter aracılığıyla ince bağırsak kolona (çekuma) bağlanır.
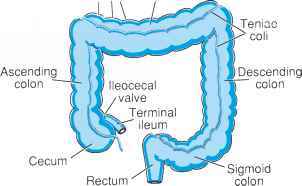
Olguların %60’ında terminal ileum tutulumu (tek başına veya diğer kolon tutulumları ile birlikte) mevcuttur. Olguların %30’unda tek başına kolit, geri kalanında ise proksimal ince barsak tutulumu görülmektedir.
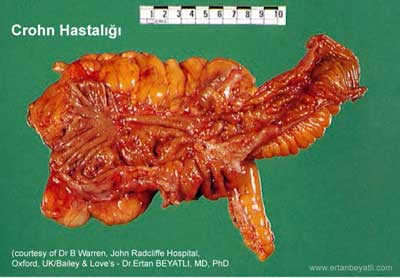
Makroskopik olarak etkilenen barsak duvarında fibrotik kalınlaşma ve lümen darlığı ve mukozada linear veya yılan tarzında ülseratif lezyonlar görülür. Ülserler arasındaki mukozanın ödemli oluşundan dolayı arnavut kaldırımı görünümü (cobblestone appearance) dikkat çekmektedir.
Transmural inflamasyon (tam kat tutulum) bu hastalığın anahtar özelliğidir ve barsak arasındaki yapışıklıklara ve fistül oluşumuna neden olur. Barsakların etkilenmeyen kısımları ise tamamen normal görünümde olur (atlama lezyonlar = skip lesions)
Belirtileri
Klinik bulgular hastalığın modeline göre değişmektedir. Çok nadir olarak Apandisit‘e benzer veya ince barsak delinmesi ve peritonit’e benzer bulgular olabilir. Bazen kolit bulguları olur.
Ancak CROHN Hastalığı ‘da en önemli durum şikayetlerin kronik (müzmin) olmasıdır. Örneğin uzun süre devam eden hafif ishal (diyare), ara ara kramp tarzında karın ağrıları, özellikle sağ alt karın köşesinde hissedilen ağrı ve dolgunluk. Aralıklı ateş, ikincil anemi ve kilo kayıp yaygın belirtilerdir. Makat bölgesinde ağrısız ülserler ve mavi renkte deri lekeleri görülebilir.
Ergenlik döneminden önce hastalığa yakalanan çocuklarda ise büyüme geriliği ve cinsel gelişim bozukluğu görülebilir.
İlerleyen durumlarda hastalığa bağlı komplikasyonlar ortaya çıkabilir örneğin barsak aralarındaki yapışıklıklar, fissür, fistül ve abse oluşumları.
Diğer bulgular: Eklem ağrıları, artrit, Göz iltihapları (üveit, iritis), Deri iltihapları (Erythema nodosum, Pyoderma gangraenosum), ağızda yara ve apse (aft), Amyloidosis, Safra kesesi taşları, böbrek taşları, Bağırsak kanseri riski, Bağırsaklarda kanama, Osteoporoz veya kemik erimesi (osteopeni), Sacroiliitis.
CROHN Hastalığı (CH) Ülserli Kolit (ÜK) arasındaki farklılıklar
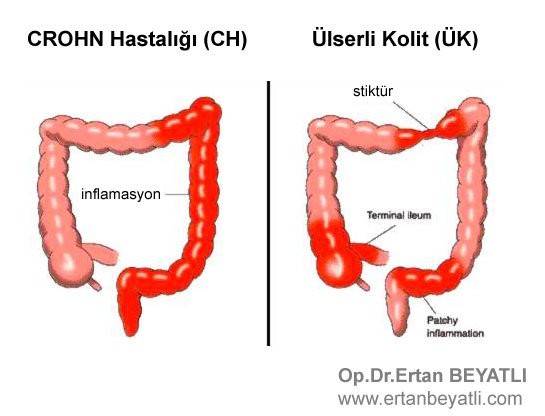
CROHN Hastalığını ülseratif kolitten ayırt etmek oldukça zor, bazı durumlarda ise imkansız olabilir.
- Ülseratif kolit kolonu etkiler; Crohn hastalığı gastrointestinal sistemin herhangi bir bölgesini etkileyebilir ancak özellikle de ince ve kalın barsak
- ÜK barsak mukozasını etkiler, CH ise tam kat olarak barsağın duvarını etkiler
- ÜK , kolon ve rektumda birleşen ülseratif lezyonlar oluşturur, CH ise atlama lezyonlar (skip lesions) ile karakterizedir.
- CH daha yaygın bir şekilde darlık (striktür) ve fistülizasyona neden olur
- CH histolojisinde Granülomlar görülebilir
- CH genellikle perianal hastalığı ile ilişkilidir
- CH terminal ileumu etkileyerek Apandisit’e benzer bulgulara neden olabilir
- Kolon ve rektum rezeksiyonu , ÜK hastasını tedavi eder, CD’de ise rezeksiyon sonrası nüks sık görülür
Tanı ve Tadavi
Hastalığın klinik bulguları doğrultusunda tanı aşamasında aşağıdaki teknikler kullanılabilir:

- Ultrasonografi (USG)
- Tam Kan ve gayta tahlili (Anemi ve GGT-gaitada gizli kan)
- Röntgen filmi ve manyetik rezonans görüntüleme (MR enteroklizis)
- Endoskopi, kolonoskopi ve biyopsi
- Bilgisayarlı tomografi ( BT)
Bazı başka hastalıklar da Crohn hastalığı benzeri belirtiler gösterebilir:
- Apandisit
- Divertikül
- Yersinia Enterocolitica enfeksiyonları
- Bağırsak tüberkülozu
- Dizanteri
- Salmonellosis gibi bulaşıcı diğer kolitler
- Gıda alerjileri ve diğer alerjiler de aşırı durumlarlarda sindirim sisteminin farklı bölgelerinde kronik iltahaplanmaya sebep olabilir ve Crohn hastalığına benzer belirtilere yol açabilir.
CROHN Hastalığı ‘nın Tedavsindeki Prensipler
- Hekim (Dahiliye Uzmanı, Gastroenteroloji) ve cerrah arasındaki yakın irtibat çok önemlidir
- Tıbbi tedavi her zaman ilk ve uzun vadeli seçenek olmalıdır. Elbette gerek görüldüğünde cerrahi uygulanabilir ancak bunun için açık ve net bir gerekçe olmalıdır, örneğin komplikasyon
- Ameliyat öncesi hastalar çok iyi ve optimize bir şekilde hazırlanmalıdır, preoperatif total parenteral beslenme gerekebilir
- CROHN Hastalığı kronik ve sık tekrarlayan bir hastalıktır, müteakip ameliyatların olasılığı açısında barsak uzunluğu, devamlılığı ve sifinkter mekanizmaları olabildiğince korunmalıdır.
CROHN Hastalığı ‘nı oluşturan sebeplerin bilinmemesi yüzünden henüz tam bir tedavi bulunmamaktadır. Hastalığın azma dönemlerinde belirtilerin ve şikayetlerin en aza indirgenmesi, mümkünse tedavisi; bu başarıldıktan sonra da remisyonun olabildiğince uzatılması şu an için geçerli olan tedavi yöntemidir.
Genelde azma döneminde bir tür steroid hormon olan glukokortikoidler ya da başka kortizonlar, salisilazosülfapiridin ya da 5-aminosalisilik asit ile birlikte kullanılır. uzun süreli kortikosteroid kullanımında ağızdan alınacak kalsiyum desteğinin ihmali, ciddi derecede osteoporoza neden olabilir. Remisyonun uzatılması ise Azathioprin gibi bağışıklık baskılayıcı ilaçlarla sağlanır. Azathioprin kullanımı sırasında da folik asit desteği ihmal edilmemelidir.
Bu ilaçların bazı durumlarda istenmeyen yan etkileri olabilir ve bunların özellikle başlangıçta doktor tarafından sık sık kontrol edilmesi gerekir.
Ameliyat ne zaman yapılmalı?
Unutulmamalıdır ki cerrahi rezeksiyon CROHN Hastalığını tedavi etmez dolayısıyla cerrahi girişim nedenlere yönelik yapılmalı ve odaklanmalıdır yani hastalığın komplikasyonları üzerinde yoğunlaşmalıdır. Agresif yaklaşan bir hekim ve konzervatif yaklaşan bir cerrah ideal tedavi için çok önemlidir.
Komplikasyonlar şunlardır :
- Tekrarlayan bağırsak tıkanıklığı
- kanama (hemoraji)
- delinme (perforasyon)
- Tıbbi tedavinin başarısızlığı
- Bağırsak fistülü
- fulminan kolit
- Malign değişiklik (kanser olasılığı)
- Perianal hastalık (makatta ülser, Anal Fistül, Anal abse, vb.)

CROHN Hastalığı ‘nda açık veya kapalı (laparoskopik) olarak çok geniş yelpazeli cerrahi yöntemler uygulanabilir.
En yaygın uygulanan cerrahi ameliyatlar şöyledir:
- ileoçekal rezeksiyon
- segmental rezeksiyon
- Kolektomi ve ileorectal anastomoz
- Subtotal kolektomi ve ileostomi
- Geçici döngü (loop) ileostomi
- proktokolektomi
- Striktüroplasti
Yorumlar kapalı.