LES gevşekliği, mide kapağı gevşekliği anlamına gelir. Normal şartlarda yiyecek ve içecekler yutulduktan sonra yemek borusu (özofagus, esophagus) aracılığı ile mideye doğru ilerletilir.
Vücudumuzun pozisyonuna göre midedeki yiyecek ve içecekler yer değiştirebilir ancak yemek borusuna geri gitmez.
İşte bu mekanizmayı sağlayan sistem Latincede LES ve Türkçesi KÖS ve AÖS olarak adlandırılır. Yutkunma refleksinin son evresinde bu mekanizma tek yönlü kapak olarak geçişe izin verir.
LES — Lower Esophageal Sphincter (alt yemek borusu kapağı)
KÖS — Kardiyo-Özofageal Sfinkter (Mide ve Yemek Borusu Kapağı)
AÖS — Alt Özofageal Sfinkter
Yani LES = KÖS = AÖS
LES Gevşekliği nasıl gelişir?
LES’in bu mekanizmasını sağlayan bir çok komplike faktör vardır. Bunların arasında
- karın ve göğüs boşluğu arasındaki zar (diyafram, diyafragma = diaphragm)
- yemek borusunun alt kısmındaki dairesel kaslar ve bazı ligamentler
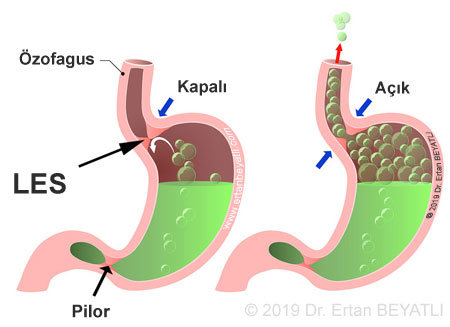
Bu mekanizmanın bozulmasında da bazı faktörler rol alır mesela karın içi basıncın artması, aşırı kilo, sigara, alkol, vb.
Ertan Beyatlı, MD, PhD
KÖS mekanizmasının bozulması mide ve yemek borusu arasındaki kapakta gevşeklik ve nadiren de olsa sıkılaşmaya neden olur.
Mide kapağı gevşekliği çok farklı şekillerde adlandırılır; örneğin LES gevşekliği, KÖS yetmezliği, LES yetersizliği, LES disfonksiyonu, AÖS yetmezliği, vb. Kapağın sıkılaşması ve aşırı kapanması durumuna ise LES Hipertonisitesi veya Kontraksiyonu denir.
LES Gevşekliği durumunda midede bulunan asit yemek borusuna doğru ilerler ve orada tahriş ve yara oluşmasına neden olur (Reflü Özofajit). Bu durum Gastro-Özofageal Reflü Hastalığı (GÖRH) olarak da bilinir.
Risk Faktörleri
Gastroözofageal Reflü Hastalığı (GÖRH) şansını arttıran bazı faktörler şöyledir:
- Obezite, Şişmanlık
- Gebelik
- Mide Fıtığı (Hiatal herni)
- Bağ dokusu hastalıkları, örneğin Skleroderma (Sistemik skleroz)
- Gecikmiş mide boşalma zamanı ve mide çıkışında darlık, örneğin pilor stenozu
- Alkol, kahve, Sigara
- Tek öğünde çok fazla yemek veya gece geç saatte yemek yemek.
- Bazı ilaçlar, örneğin aspirin
LES Gevşekliği Belirtileri
KÖS Gevşekliği yaşayan hastalarda aşağıdaki belirtiler görülebilir:
- midede yanma, ekşime
- yemek borusunda yanma, göğüste yanma ve ağrı
- ağza acı su gelmesi
- ilerleyen durumlarda bulantı, kusma, kilo kaybı
- ağrılı yutkunma, odinofaji
- boyunda veya boğazda gıcık hissi
- nedeni bulunamayan Kronik öksürük
- faranjit, larinjit
- Astım benzeri şikayetler
- Uyku bozukluğu
LES Gevşekliği veya GÖRH Tanısı
Sizi takip eden doktor, şikayetleriniz ve hikayenize doğrultusunda yapacağı fiziki muayene sonrası tanıyı koyabilir.
Konulan teşhisi destekleme babında ve komplikasyonların olup olmadığını kontrol etmek amacıyla doktorunuz bazı testleri isteyebilir, örneğin:
- Endoskopi (Gastorskopi) (bkz: Endoskopi uyutularak nasıl yapılır?)
- Ambulatuvar asit (24 saat pH) prob testi. Bu testte yemek borusunun alt kısmına bir prob yerleştirilir. Böylelikle 24 saat içerisinde asid reflüsünün zamanı ve miktarı ölçülür. İki çeşit prob vardır. İlkinde prob çok ince bir kablo ile üzerinizde taşıyacağınız bir alıcıya bağlıdır. İkincisinde ise prob kablosuzdur ve kendiliğinden 1-2 gün içerisinde düşüp dışkıyla atılır.
- Özofagus manometrisi. Bu test, yutulduğunda yemek borunuzdaki ritmik kas kasılmalarını ölçer. Özofagus manometrisi, özofagus kaslarının uyguladığı koordinasyonu ve kuvveti de ölçer (özofagus barometrik ölçüm).
- Üst sindirim sisteminizin röntgeni (X-ray). ÖMD-Baryum grafisi
Komplikasyonlar
Tedavi edilmediğinde, devam eden yemek borusu iltihabı zamanla bazı sorunlara yol açabilir:
- Yemek borusunun daralması (özofagus darlığı). Mide asidinin alt özofagusa zarar vererek skar dokusunun oluşmasına neden olur. Yara dokusu yiyecek yolunu daraltarak yutma problemlerine yol açar.
- Yemek borusunda açık bir yara (özofagus ülseri). Mide asidi yemek borusundaki dokuyu aşındırabilir ve açık bir yara oluşmasına neden olabilir. Bir özofagus ülseri kanama ve ağrıya neden olabilir ve yutmayı zorlaştırabilir (disfaji, odinofaji)
- Yemek borusunda kanser öncesi değişiklikler (Barrett’s özofagus mukozası). Asit hasarı, zaman ilerledikçe alt özofagusu kaplayan dokuda değişikliklere neden olabilir. Bu değişiklikler özofagus kanseri riskinde artış ile ilişkilidir.
Ayrıca uzun vadede astım, kronik öksürük ve solunum şikayetleri gelişebilir. Diş, diş eti ve ağı içi sorunlar da baş gösterebilir.
LES Gevşekliği Tedavisi

LES Gevşekliği için birçok tedavi ve cerrahi girişim seçeneği mevcuttur. Tedavinin asıl amacı yemek borusuna giden asidi azaltmak ve kapak mekanizmasını onarmaktır (Anti-Reflü Yöntemler, örneğin fundoplikasyon).
Doktorunuzun ilk önce yaşam tarzı değişikliklerini ve reçetesiz satılan ilaçları denemenizi tavsiye etmesi olasıdır. Birkaç hafta içinde rahatlama yaşamazsanız, doktorunuz reçeteli ilaç veya ameliyat önerebilir.
İlaçların Mekanizması
- Mide asidini nötralize eden antasitler.
- Asit üretimini azaltan ilaçlar. (H2 reseptör blokerleri)
- Asit üretimini bloke eden ve yemek borusunu iyileştiren ilaçlar. (Proton Pompa İnhibitörleri)
Diyet — Bazı hastalarda bazı yiyecekler şikayetleri tetikleyebilir ve bu yiyeceklerden uzak durmaları lazım. Örneğin: yağlı ve baharatlı yiyecekler, çikolata, narenciye, Ananas, domates, soğan, Sarımsak, nane, alkol, Kahve, Çay ve soda.
Şikayetleri azaltmak için evde bazı önlemler alınabilir. Örnein:
- Sigarayı bırakmak
- aşırı kilolardan kurtulmak
- az az sık sık yemek
- yedikten sonra sakız çiğnemek, uzanmaktan kaçınmak
- belirtilerinizi tetikleyen yiyecek ve içeceklerden kaçınmak
- dar kıyafetler giymekten kaçınmak
- rahatlama egzersizleri uygulamak
Bazı bitkisel ilaçlar da rahatlama sağlayabilir. GÖRH için yaygın olarak kullanılan otlar şunlardır:
- sarı papatya
- meyan kökü
- hatmi kökü
- kaygan karaağaç
Cerrahi ve diğer işlemler
GÖRH ve LES Gevşekliği genellikle ilaçla kontrol edilebilir. Ancak ilaçlar yardımcı olmazsa veya uzun süreli ilaç kullanımından kaçınmak istiyorsanız doktorunuz size bazı cerrahi girişimler önerebilir:
Fundoplikasyon ameliyatı

Bu ameliyat esnasında, midenin üst kısmı sfinkter mekanizmasını güçlendirmek, asit reflüsünü önlemek ve hiatal herniyi onarmak için LES etrafına sarılır. Fundoplikasyon genellikle minimal invaziv (laparoskopik) bir prosedürle yapılır. Midenin üst kısmının sarılması kısmi (Toupet) veya tam (Nissen) olabilir.
Manyetik Sfinkter Güçlendirme Cihazı (LINX cihazı)

Mide ve yemek borusunun birleşme yerinin etrafına küçük bir manyetik boncuk halkası sarılır. Boncuklar arasındaki manyetik çekim, birleşme noktasının geri akıştaki aside kapalı kalmasına yetecek kadar güçlüdür, ancak gıdaların geçmesine izin verecek kadar zayıftır. Linx cihazı minimal invaziv cerrahi (laparoskopi) kullanılarak yerleştirilebilir.
Gebelik ve GÖRH
Hamilelik asit reflü yaşama şansınızı artırabilir. Hamilelik sırasındaki hormonal değişiklikler yemek borunuzdaki kasların daha sık gevşemesine neden olabilir. Büyüyen bir fetüs de mideniz üzerinde baskı yaratabilir. Bu, mide asidinin yemek borunuza girme riskini artırabilir.
Asit reflü tedavisinde kullanılan birçok ilaç hamilelik sırasında güvenlidir. Ancak bazı durumlarda doktorunuz bazı antasitler veya diğer tedavilerden kaçınmanızı önerebilir. Gebelikte asit reflü’nü yönetmek için kullanabileceğiniz stratejiler hakkında daha fazla bilgi edinin.
IBS ve GÖRH
İrritabl barsak sendromu (IBS) kalın bağırsaklarınızı etkileyebilecek bir durumdur. Yaygın semptomlar: karın ağrısı, şişkinlik, kabızlık, ishal. Yakın tarihli bir incelemeye göre, GÖRH ile ilişkili semptomlar IBS’li insanlarda genel popülasyondan daha yaygındır.
Alkol içmek ve GÖRH
GÖRH’li bazı insanlarda, bazı yiyecek ve içecekler semptomları daha da kötüleştirebilir. Bu diyet tetikleyicileri alkollü içecekler içerebilir.
Özel tetikleyicilerinize bağlı olarak, ölçülü olarak alkol içebilirsiniz. Ancak bazı insanlar için, az miktarda alkol bile GÖRH semptomlarını tetikler.
Alkolü meyve suları veya diğer karıştırıcılarla birleştirirseniz, bu karıştırıcılar da belirtileri tetikleyebilir. Alkol ve mikserlerin GÖRH semptomlarını nasıl tetikleyebileceğini keşfedin.

Hocam özofajit AÖS gevsekligi Pangastrit nedir tanı olarak kocama bunu yazmışlar bugu
mide kapağında gevşeklik demektir. pangastrit için burdaki makaleme bakabilirsiniz PANGASTRİT ve ANTRAL GASTRİT