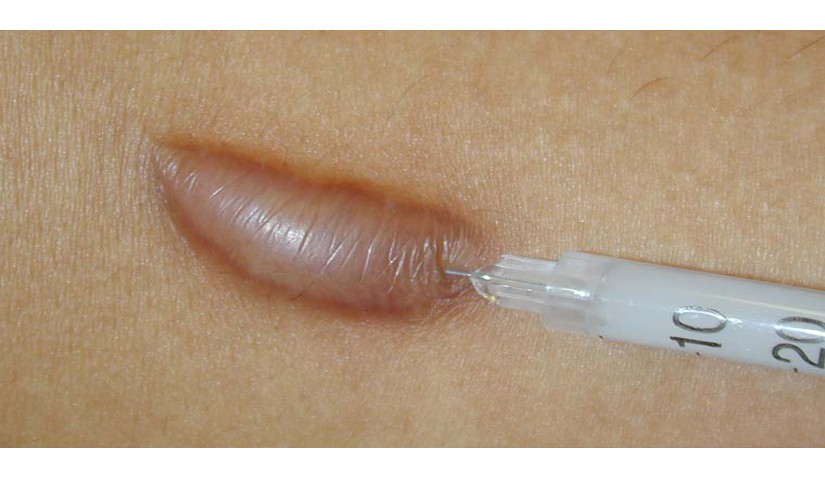
Keloidler genellikle cilt yaralanmasının iyileşmesinden sonra gelişen yoğun fibröz dokunun aşırı büyümesinin sonucudur. Dokusu orijinal yaranın sınırlarını aşar, genellikle kendiliğinden gerilmez ve eksizyondan sonra tekrarlama eğilimi gösterir.
Keloid (papirüs üzerine kaydedilen) ilk açıklaması M.Ö. 1700’de Mısır’da kullanılan cerrahi tekniklerle ilgilidir. Ardından, 1806’da Alibert, dokunun etkilenmemiş deriye yanal gelişimini tanımlamak için Yunan chele’sinden veya yengeç pençesinden türetilen terimi kullandı.
Hipertrofik Skar nedir?
Keloidun aksine, hipertrofik yara izleri tipik olarak ilk hasarın sınırlarını aşmayan eritemli, pruritik, yükseltilmiş fibröz lezyonlarla karakterizedir ve kısmi spontan çözünürlüğe uğrayabilir. Hipertrofik yara izi, derin deri tabakasının (dermis) bulunduğu termal yaralanmalar ve diğer yaralanmalar sonrasında yaygındır.
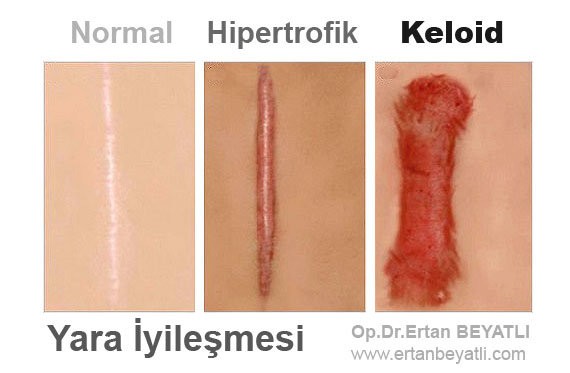
Keloidler nadiren kendiliğinden düzelir; Bununla birlikte, tedavi ile yumuşak ve daha az ağrılı ve pruritik hale gelebilirler. Tek başına eksizyon tedavisi takiben, keloidler tekrar tekrar ortaya çıkar (>% 50).
Çoğu yerde bulunan keloidler ve hipertrofik yara izleri öncelikle kozmetik açıdan rahatsızlık verir. Bununla birlikte, bazı keloidler veya hipertrofik yara izleri kontraktürlere neden olabilir ve bu da önemli bir şekil bozukluğuna neden olabilir.
Keloidler ve hipertrofik yara izleri genetik olarak HLA-B14, HLA-B21, HLA-Bw16, HLA-Bw35, HLA-DR5, HLA-DQw3 ve kan grubu A ile ilişkilidir.
Keloidler ve hipertrofik skarlar genellikle semptomlara neden olmaz, ancak bazen ağrılı veya kaşıntılı olabilir veya yanma hissine neden olabilirler. Semptomatik rahatlamaya ek olarak, kozmetik kaygı, hastaların tıbbi müdahale talep etmesinde başlıca nedendir.
Keloid Lezyonların kaynağı
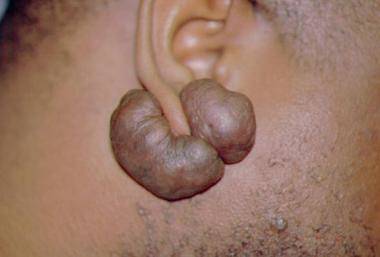
Keloidler travma dokusunun abartılı büyümesi olarak, genellikle travma öncesi bölgelerde ortaya çıkar. Keloidler çevresindeki cilt seviyesinin üstünde uzanan travma alanlarını aşar ancak subkutanöz dokuya nadiren uzanırlar.
Hipertrofik yara izleri travmatik bölgeyle sınırlı kalırken, 12-24 ay içinde kendiliğinden gerileyebilir.
Klinik Bulgular
Keloidler yumuşak ve elastik yapıdadır. Erken lezyonlar genellikle eritematözdür. Lezyonlar kahverengimsi kırmızıya dönüşür ve yaşlandıkça soluklaşır. Lezyonlar genellikle saç kökü ve diğer işleyen adneksiyel bezlerden yoksundur.
Lezyonlar oluştuğunda klinik seyir değişir. Çoğu lezyon, haftalarca aylarca ve diğerleri yıllarca büyümeye devam eder. Büyüme genellikle yavaş, ancak keloidler bazen hızla büyür ve aylar boyu üç kat artar. Büyümeyi bıraktıklarında, keloidler genellikle semptomlara neden olmaz ve kararlı kalır veya hafifçe çekilir.
Kulak, boyun ve karın üzerindeki keloidler kabarma (pedunkülasyon) eğilimi gösterir. Merkezi göğüs ve ekstremitelerdeki keloidler genellikle düz bir yüzeye kaldırılır ve taban genellikle üstten daha geniştir.
Çoğu keloid yuvarlak, oval veya düzenli kenar boşluklarıyla dikdörtgen şeklindedir; Bununla birlikte, bazılarının düzensiz sınırları olan tırnağa benzer yapıları vardır. Eklemde oluşan keloidler hareketi kısıtlayabilir.
Çoğu hastada 1 veya 2 keloid görülür; Bununla birlikte, birkaç hastada, özellikle de spontan keloid hastalarında çok sayıda lezyon vardır ve sivilce veya suçiçeği nedeniyle keloid geliştiren hastalar da vardır.
Keloidler, hipertrofik yara izinden, hipertrofik yara izi içinde bulunmayan pençe benzeri (clawlike) projeksiyonlardan ayırdedilebilirler.
Lezyon alanlarının sıklığı
Açık renkli insanlarda keloidler, yüzün (yanak ve kulak memeleri baskındır) azalan sırayla, üst ekstremitede, göğüs, ön bölge, boyun, sırt, alt ekstremite, göğüs ve karında eğilim gösterir.
Koyu renkli insanlarda, frekansın azalan sırası kulak memeleri, yüz, boyun, alt ekstremiteler, göğüsler, göğüs, sırt ve karın eğilimi gösterir.
Asya kökenli insanlarda frekansın azalan sırası kulak memeleri, üst ekstremiteler, boyun, göğüsler ve göğüstür.
Keloid ve Hipertrofik yara Nedenleri
Aslında nedeni bilinmemektedir. Artmış kutanöz pigmentasyona paralel olarak artan keloidlerin yaygınlığı, genetik bir temeli veya en azından bir genetik bağlantı olduğunu düşündürmektedir.
Keloidlerin gelişimi için belirlenen birincil nedeni, cilt için hem travma hem de patolojik (örn., Kulak tıkanıklığı, cerrahi) ve patolojik (örn. Sivilce, su çiçeği). Yabancı madde, enfeksiyon, hematom veya artmış cilt gerginliği varlığında duyarlı bireylerde keloid veya hipertrofik skar oluşumuna neden olabilir. Transforman büyüme faktörü-beta ve adiponektin patogenezde rol oynar.
Keloid için Tıbbi bakım
Tüm keloidler için en iyi tedavi yöntemi diye birşey yoktur. Lezyonun yeri, büyüklüğü ve derinliği; hastanın yaşı; ve tedaviye olan geçmiş cevap, kullanılan terapi türünü belirler.
Önleme önemlidir, ancak hipertrofik skarların ve keloidlerin terapötik tedavisi, tıkayıcı pansumanlar, kompresyon tedavisi, intralezyonel kortikosteroid enjeksiyonları, kriyocerrahi, eksizyon, radyasyon terapisi, lazer terapisi, IFN terapisi, 5-fluorourasil (5-FU), doksorubisin, tamoksifen, takrolimus, botulinum toksini, hidrojel iskele ve reçetesiz tedaviler (örneğin soğan ekstraktı, hidrokortizon, silikon ve vitamin E kombinasyonu).
Diğer vaat eden tedaviler, vasküler endotelyal büyüme faktörü (VEGF) inhibitörleri (örneğin bevacizumab), fototerapi (fotodinamik terapi [PDT], UVA-1 tedavisi, dar bant UVB tedavisi), transforme edici büyüme faktörü (TGF) -beta inhibitörlerini içeren antiangiogenik faktörleri, kolajen sentezini düşürmeye yönelik tümör nekroz faktörü (TNF) -alpha inhibitörleri (etanersept), rekombinant insan epidermal büyüme faktörü (rhEGF) ve rekombinant insan interlökin (rhIL) -10’dur.
Keloid Önlenebilir mi?
Keloid terapisinde ilk kural önleme yöntemidir. Keloid oluşturduğu bilinen hastalarda gereksiz kozmetik cerrahi yapmaktan uzak durması önemli bir husustur. Bu insanlarda yapılacak cerrahi müdahalelerde dokulara çok minimal düzeyde travma yapılmalı ve ameliyat sonra yara bakımı ve takibi yapılmalıdır.