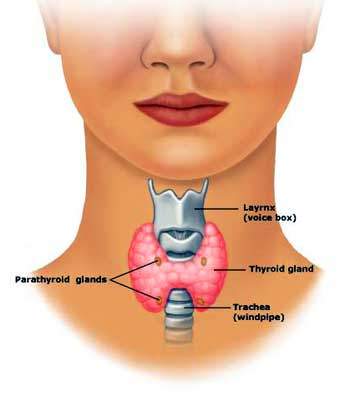
Guatr (Goiter), tiroit bezinin büyümesidir. Normal troit bezinin ağırlığı 20-25 gm ve boyutları 20 x 25 x 50 mm’dir.
Ele gelen her tiroit bezi guatr olarak değerlendirilemez ancak ultrasonografik ölçümle kesin tanı konmalıdır. Ultrasonografide tiroit bezinin derinlik çapı 25mm üzerine ise guatr tanısı konulabilir.
Guatr Çeşitleri
Guatrın çeşitli sınıflaması vardır. Tiroit bezinin hormon üretme durumuna göre 3 ana sınıfa ayrılır:
- Ötiroidi : hormonlar normal düzeylerdedir
- Hipotiroidi : hormonlar azalmıştır
- Hipertiroidi: hormonları yükselmiştir
Tiroit nodülü nedir?
Tiroit bezinde oluşan kitledir. Nodüller kistik, solid ve miks durumda olurlar. Kistik nodül içinde sadece sıvı, Solid nodüller hücrelerin büyümesi ve çoğalması, Miks nodüller ise içerisinde kistik ve solid bölümleri olan nodüllerdir. (bkz, Tiroid Nodülleri)
Guatr belirtileri nelerdir ?
- Hipotiroidi (Tiroid bezinin az çalışması); yorgunluk, halsizlik, uyuşukluk, uyku hali, konsantrasyon bozukluğu, sersemlik hissi, depresyon, saç dökülmesi, ciltte kuruma ve soğukluk hissi, kabızlık, kilo alma, göz kapakları ve bacaklarda şişlik, terlemede azalma, balmumu gibi cilt, soğuğa tahammülsüzlük, üşüme, ses kalınlaşması, ses kısılması, konuşmada ağırlaşma, reflekslerde azalma, tansiyon, kolesterol yüksekliği ve nabız düşüklüğü, adet düzensizliği, hamile kalmada zorluk, çocuklarda boy kısalığı ve gelişme geriliği gibi belirtilerle kendini gösterir.
- Hipertiroidi (Tiroid bezinin çok çalışması) ise; sinirlilik, aşırı heyecan, duygusallık, kilo kaybı, terleme ve vücut sıcaklığında artma, ellerde titreme, nabız sayısında ve tansiyonda artış, cilt terleme ve nemlilik hissi, saç dökülmesi, sıcağa tahammülsüzlük, bağırsak hareketlerinde artma, adet düzensizliği, gözde canlı bakış, bazen tek gözde büyüme, bazen çift görme şeklinde ortaya çıkar.
Guatrın teşhisi nasıl konur?
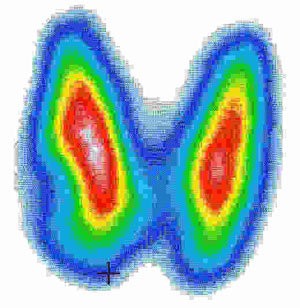
Guatr teşhisi; muayene, kan testi (T3, T4, TSH hormonları tetkiki), tiroid ultrasonu veya tiroid sintigrafisi ile konur.
Guatrın tedavi yöntemleri nelerdir?
Tedavi yöntemleri; ilaç tedavisi, radyoaktif iyot tedavisi ve cerrahi tedavidir. Tedavi yöntemlerinden hangisi veya hangilerinin seçileceği hastadan hastaya değişir. En uygun tedavi şeklinin cerrah, endokrinolog, radyolog ve patologdan oluşan bir ekip tarafından planlanması ve takip edilmesi gerekir.
Tiroidektomi Çeşitleri
- Hemithyroidectomy
- Subtotal thyroidectomy
- Partial thyroidectomy
- Near total thyroidectomy
- Total thyroidectomy
- Hartley Dunhill operation

Tiroid Cerrahisi Çeşitleri
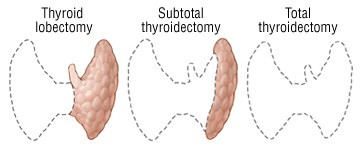
Üç ana tiroid ameliyatı vardır:
- Tiroid lobektomi (Thyroid lobectomy)
- Total veya totale-yakın tiroidektomi (Total or Near-total thyroidectomy)
- Tiroidektomi Tamamlaması, Tamamlayıcı Tiroidektomi (Completion thyroidectomy)

Tiroid lobektomi
Bu ameliyat nodülü olan tiroid bezinin yarısını almayı içerir. Bazen “tanısal lobektomi ” olarak adlandırılır, çünkü ameliyat öncesi (preoperatif) tanı belirsiz olabilir ve ameliyatın nedeninin bir kısmı kanser teşhisi koyma amaçlıdır. Bu hastalarda iğne (TİİAB, FNA) biyopsi sonucu, tanısal olmayan, malignite için şüpheli olan veya bir foliküler veya Hurthle hücre neoplazmı gösteren türdedir.
Tanısal lobektomi donmuş bir bölüm (Forezn) içerebilir veya içermeyebilir. Donmuş bir kesit, hasta hala anestezi altında iken operasyon sırasında alınan nodülün biyopsisidir. Patolog mikroskop altında tiroid nodülünün bir veya iki dilimini inceler ve tanı koymaya çalışır. Donmuş kısımda kesin kanser bulunursa, o zaman hastanın total tiroidektomi ameliyatına karar verilir. Donmuş bölümün %100 doğru olmadığına dikkat etmek önemlidir. Patolog nodülün sadece bir veya iki dilimine baktığından, incelenen dilimlerde değil, kanser kanıtı olma olasılığı yüksektir. Patolog, daha sık olmamak üzere, foliküler veya Hurthle hücre kanseri teşhisini donmuş bölüm üzerinde yapamaz ve nihai patolojinin (özel işlem gerektiren ve tüm numunenin incelenmesine izin veren kalıcı bölümler) beklenmesi gerekir. Son patoloji genellikle ameliyattan yaklaşık 5-7 iş günü sonra hazır olur. Donmuş kısımda kanser bulunmazsa, ancak son patolojide bulunursa, tiroid bezinin geri kalanını çıkarmak için ikinci bir ameliyat gerekebilir (tamamlayıcı tiroidektomi veya Tiroidektomi tamamlaması ). Sonuçta, donmuş bir bölümün gönderilip gönderilmemesi cerrahın deneyimine ve uzmanlığına bağlı olacaktır.
Tiroid bezinin yarısı alınmış tüm hastaların ameliyattan bir süre sonra tiroid seviyelerini kontrol ettirmeleri gerekecektir. Bu seviyelere bağlı olarak, bazı hastalar tiroid hormon replasmanına ihtiyaç duyabilir ve bazı hastalar da gerekmez.
Total veya totale-yakın tiroidektomi
Bu ameliyat tiroid bezinin tamamını ya da neredeyse tamamını çıkarmayı içerir. Büyük guatr veya Graves ‘hastalığı tiroid loblarını etkileyen iyi huylu tiroid koşulları için yapılabilir veya kanser için yapılabilir. Totale-yakın tiroidektomi, cerrahın arkasında çok az miktarda benign tiroid dokusu bırakmaya karar verdiği anlamına gelir. Tiroid dokusu, sesi kontrol eden, yutma ve nefes alma gibi sinirler veya paratiroid bezleri gibi önemli yapıların çevresindeki alanlarda kasıtlı olarak geride kalabilir. Total veya totale yakın bir tiroidektomi yapılan tüm hastaların ameliyat sonrası yaşam boyu tiroid hormon replasmanında olması gerekir.
Tiroidektomi Tamamlaması (Tamamlayıcı tiroidektomi)
Tamamlama tiroidektomi, bir hasta önceden kısmi (parsiyel) tiroid rezeksiyonu geçirdikten sonra (yani lobektomi) kalan tiroid dokusunu çıkarmayı içerir. Yıllar sonra yapılabilir veya lobektomiden kısa bir süre sonra yapılabilir (bir sonraki hafta kadar erken). Tiroidektominin tamamlanma nedenleri lobektomi veya total tiroidektomi ile aynıdır. . Tamamlayıcı tiroidektomi uygulanan tüm hastaların ameliyat sonrası yaşam boyu tiroid hormon replasmanında olması gerekir.