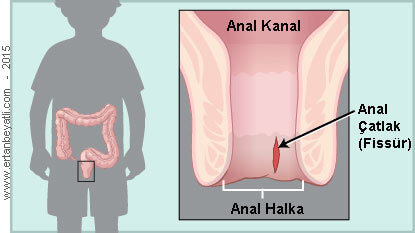
Anal Fissür oturak bölgesinde (anüs, makat veya anoderm) uzunlamasına oluşan yırtıklar veya çatlaklardır. Yırtıklar dış kısımdan içe doğru uzanır ancak dentate çizgisini geçmez. En yaygın nedenleri ise kabızlık, ıkınma, doğum ve düzensiz beslenme alışkanlıklarıdır.
Halk arasında bu hastalığın adı çoğu zaman yanlış bir şekilde telaffuz edilebilir; örneğin fistür hastalığı, fikstür hastalığı, fixtur hastalığı ve firsür hastalığı şeklinde. Doğru yazılış şekli ise “Anal Fissür” dür.
Ayrıca Anal Fissür insanlar arasında sıklıkla Anal Fistül ile karıştırılır. Bu iki hastalığın sadece isim benzerliği vardır ve tamamen ayrı durumları ifade eder. Fissür, çatlak veya yırtık demektir, fistül ise kanal veya tünel demektir.
Anal Fissür’ün Nedenleri
Fissürün nedenleri şunlardır:
- Büyük veya sert dışkılama
- Kabızlık, ıkınma ve zorlanma
- Kronik ishal
- Çocuk doğurma, gebelik
- Diğer: Crohn hastalığı, inflamatuar bağırsak hastalığı, Anal kanser, HIV, Tüberküloz (verem), anal ilişki ve Frengi
Anal Fissür’ün Belirtileri
Şikayetler hastalığın süresi ve kişinin ağrı eşiği durumuna göre değişebilir:
- Makat ağrısı. Özellikle dışkılama esnasında başlayan ağrı 1-8 saat giderek azalan bir şekilde devam eder, bazen gün boyu devam edebilir.
- Makatta meme oluşması.
- Makatta kaşıntı.
- Makatta kanama. Dışkılama esnasında ve sonrasında az miktarda açık pembe kan çizgileri görülebilir.
- Makatta yanma. Çatlak bölgesindeki sinirlerin açıkta kalmasından kaynaklanır, erken dönemde daha belirgindir.
- Camla çiziliyormuş hissi. Dışkının makattan geçerken çatlakta yaptığı sürtünmeyle oluşur.
- Zor dışkılama. Çatlak sebebiyle makat kaslarının gevşemesi zorlaşır ve yeterince gevşeyemez buna bağlı olarak dışkıyı çıkarmak için daha çok ıkınmak gerekir.
- Kabızlık. Hasta ağrı olacak korkusuyla dışkılama ihtiyacının erteler buna bağlı olarak barsakta bekleyen dışkının suyu daha fazla emildiği için katılaşır.
- Karında şişkinlik. Dışkıyı ertelemek ve makat basıncının yükselmesi sebebiyle barsakta biriken gaz ve dışkı miktarı artar.
- Makatta darlık. Makat kaslarının kontrolsüz bir şekilde kasılması fonksiyonel bir darlık gibi algılanır. Gerçek bir darlık değildir fissür düzeldiğinde kendiliğinden geçer
- İdrarda yanma hissi. Seyrek görülen bir durumdur makattaki hislerin idrar yollarına yansıması sebebiyle görülür.
Çeşitleri
Anal Fissürlerin süresine göre başlıca iki çeşidi vardır:
- Akut Anal Fissür. Süresi bir aydır. Aşırı ağrı ve pembemsi akıntı veya çok az miktarda kanama görülebilir.
- Kronik Anal Fissür. Bir aydan daha fazla devam eden çatlaklar Kronik Anal Fissür olarak adlandırılır. Kronik fissürlerde ağrı oranı daha az ve bazen ağrısız kanamalar meydana gelebilir. Bu durumda makat bölgesinde meme şeklinde koruyucu bir deri uzantısı oluşur. Bu memenin adı “Skin Tag” veya “Bekçi nodül pile” dır. Latincesi anal papilla hipertrofisidir. Bu durum çoğu zaman basur (hemoroid) ile karıştırılır ve yanlış tanıya ve dolayısıyla yanlış tedaviye neden olur.
Anal Fissür Tedavisi
Akut anal fissürlerin tedavisi ilaçla gerçekleşebilir. Barsak alışkanlıklarını düzenleyen çeşitli ilaçlar ve makat bölgesine sürülen farklı lokal kremler ve fitiller mevcuttur (makat çatlak kremi). Kronik anal fissürün için cerrahi müdahale ve lazer tedavi seçeneği mevcuttur.
Sfinkterotomi ve Fissürektomi
Lokal anestezi altında makat bölgesinin istemsiz olarak büzüşmesine yol açan sfinkter kasları elektrokoter yardımı ile diseke edilir (Lateral internal sfinkterotomi LİS). Gerekirse fissür zemini koter ile eksize edilir ve yakılır (Fissürektomi) . Meme mevcutsa çıkartılır.
Bu operasyonun süresi ortalama 15-30 dakikadır. Hasta müdahaleden sonra mobilize olup evine dönebilir. Müdahale sonrası çeşitli ilaçlar verilir ve 4-5 güne kadar ılık su oturma banyosu önerilir. Hasta 24 saat sonra işbaşı yapabilir.
Cerrahi müdahaleden sonra bazı komplikasyonlar meydana gelebilir örneğin: kanama, hematom, enfeksiyon, gaz veya dışkı kaçırma.
Anal ilerleme Flepleri
Anal ilerletme flepleri, anal astarından sağlıklı bir mukoza almayı ve fissürü örtmek için kullanmayı içerir. Sağlıklı mukoza dikişlerle yerine tespit edilir. Bu prosedür çok sık yapılmamaktadır. Sfinkterotomi ile aynı anda veya daha sonra fissür hala iyileşmiyorsa bu yönteme başvurulabilir. Ameliyattan sonra dışkı kaçırma (inkontinans) gelişme riskiniz daha yüksekse de bir seçenek olabilir.
Lazerle Anal Fissür tedavisi
Yeni nesil lazer cihazları (Neolazer) aracılığıyla anal fissür zemini kurutulur. Bu sayede ameliyat riskleri ve komplikasyonları ortadan kaldırılmış olur. Neolazer işlemi lokal, spinal veya genel anestezi ile yapılabilir ve ortalama süresi 5-10 dakikadır. İşlemden sonra hasta işine veya evine dönebilir. Çoğu hastada fissürle birlikte hemoroid memeleri de eşlik eder. Bu durumlarda lazer tedavisi daha konforlu bir seçenek olarak karşımıza çıkmaktadır.
Detaylı bilgi için:
Op. Dr. Ertan Beyatlı Klinik
Karakaş Mah., Fevzi Çakmak Blv., No:34, D:1, 39000 Kırklareli/Türkiye
Tel: +90 531 618 8964
Ayrıca Lazerle Hemoroid tedavisi için buradaki makaleme bakabilirsiniz: Lazerle Hemoroid tedavisi
Tedaviye karar vermek
Anal fissür hakkında doktorunuzla ilk kez görüştüğünüzde, sizinle birlikte olası tedavi seçeneklerinden geçecek ve neyin dahil olduğunu anladığınızdan emin olacaklardır. Belirli bir prosedür öneriyorlarsa, öncesinde, sırasında ve sonrasında ne olacağını ve sahip olabileceğiniz olası komplikasyonları tartışacaklardır.
Bu, neler olacağını anlamanız için soru sorma fırsatınızdır. Kremler ve merhemlerle daha fazla tedaviye devam etmeyi tercih edebilirsiniz. Bir prosedüre devam etmeye karar verirseniz, bir onam formu imzalamanız istenir (bazen anlaşma formu da denir).
Prosedürden önce yemeyi ve içmeyi ne zaman bırakacağınız ve o gün ne olacağı gibi uymanız gereken bilgiler ve talimatlar verilecektir.


Yorumlar kapalı.